This guide explains the basics so they can arrive confident, avoid common mistakes, and get the most useful data from their study.
What is a sleep test, and why might someone need one?
A sleep test Brisbane clinic may recommend a test that records breathing, oxygen levels, heart rate, and sleep patterns to check for disorders like obstructive sleep apnoea. Many patients are referred after snoring, choking or gasping at night, or ongoing daytime fatigue.
Clinicians also recommend testing when there is high blood pressure, morning headaches, poor concentration, or a partner notices breathing pauses.
What types of sleep tests are available in Brisbane?
Most first-time patients are offered either an at-home sleep study or an in-lab overnight study (polysomnography). The right option depends on symptoms, health history, and how complex the suspected issue is.
At-home tests are common for straightforward suspected sleep apnoea. In-lab studies can capture a wider range of signals and are often used when results need deeper analysis.
How does an at-home sleep test work?
In an at-home study, they take home a small device with sensors, wear it overnight, then return it the next day. The setup usually includes a finger probe for oxygen, belts around the chest or abdomen, and a nasal cannula to measure airflow.
Most patients can sleep in their own bed, which often helps them sleep more naturally than they would in a clinic.
What happens during an in-lab sleep study?
In a sleep lab, they sleep overnight while a technician monitors signals in real time. The setup typically includes sensors on the scalp, face, chest, and legs, plus airflow and oxygen monitoring.
The room usually looks like a simple hotel-style bedroom. The goal is to capture enough normal sleep to measure breathing events, arousals, and sleep stages accurately.
How should first-time patients prepare for their sleep test?
They should follow their normal routine as much as possible, unless the clinic gives different instructions. Patients usually get the best results when they aim for a typical night rather than trying to “sleep perfectly.”
Common preparation steps include avoiding naps late in the day, limiting caffeine after lunchtime, and packing comfortable sleepwear if attending an overnight lab.
What should they bring for an overnight sleep test?
They should bring toiletries, nightwear, and any items that help them sleep, such as a pillow if permitted. Patients who use medications should bring them and take them as directed, unless instructed otherwise.
It also helps to bring a list of current medications and any relevant health notes, especially if they have asthma, heart conditions, or chronic nasal congestion.
Will the sleep test be uncomfortable or painful?
A sleep study is not painful, but some patients find the sensors mildly annoying at first. Most adjust within minutes and fall asleep normally once lights are off.
If they are worried about sensitivity to tape or adhesives, they can tell the clinic beforehand so staff can use alternative materials where possible.
What if they cannot sleep on the night of the test?
Most studies still work even if they sleep less than usual. Clinicians typically need a minimum amount of recorded sleep time to interpret breathing and oxygen patterns reliably.
If they barely sleep, the clinic may recommend repeating the study. Patients should not try to “force” sleep; staying calm usually leads to better results than stressing about the clock.
How long does a sleep test take, and when do results come back?
The recording is usually one night, though some home studies may be repeated if data quality is poor. After the device is returned, the data is analysed and a report is prepared for the referring doctor or sleep specialist.

Turnaround times vary, but many patients receive results within one to two weeks, depending on clinic workload and whether specialist review is required. Click here to get about Perth sleep study cost: public vs private comparison guide.
What do the results typically show?
Results often include an index of breathing disruptions, oxygen drops, and snoring patterns, plus an overall severity rating if sleep apnoea is found. They may also highlight sleep position effects, such as worse breathing when lying on the back.
If an in-lab study is done, the report can include sleep stages and limb movement data, which can help identify other sleep disorders.
What happens if they are diagnosed with sleep apnoea?
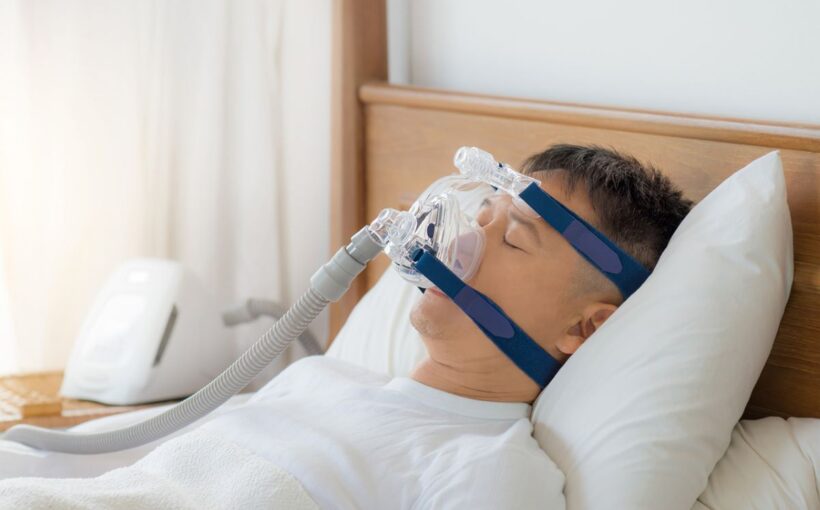
If sleep apnoea is confirmed, the next step is usually a treatment discussion based on severity, symptoms, and personal preferences. Many patients are offered CPAP therapy, which uses gentle air pressure to keep the airway open.
Other options may include mandibular advancement devices, weight management strategies, positional therapy, nasal treatments, or referral for further assessment if anatomy plays a major role.
How can they avoid common mistakes that affect results?
They should ensure sensors are fitted correctly and follow the written instructions closely for home tests. Many failed studies happen because the nasal cannula slips out, belts are too loose, or the device is not turned on.
They should also report unusual factors, like alcohol intake, illness, or severe congestion, because those can change breathing and may affect how results are interpreted.
What questions should they ask the clinic or doctor beforehand?
They should ask which test type is being used, what it measures, and what happens if results are borderline. It also helps to ask about costs, rebates, and whether a follow-up appointment is included.
If they have special needs, they should ask about accessibility, allergies, anxiety around testing, and whether a support person can attend if it is an in-lab study.
What should they do next if they still feel tired after a “normal” result?
A normal test does not always mean nothing is wrong; it may mean sleep apnoea was not the cause. They should return to their GP or sleep specialist to discuss other possibilities such as insomnia, restless legs, circadian rhythm issues, medication effects, depression, or thyroid and iron problems.
In some cases, a different type of study or repeat testing is recommended if symptoms remain strong.
FAQs (Frequently Asked Questions)
What is a sleep test and why might I need one in Brisbane?
A sleep test records breathing, oxygen levels, heart rate, and sleep patterns to check for disorders like obstructive sleep apnoea. You might be referred for a test if you experience snoring, choking or gasping at night, ongoing daytime fatigue, high blood pressure, morning headaches, poor concentration, or if a partner notices breathing pauses.
What types of sleep tests are available in Brisbane and which should I choose?
In Brisbane, you can have either an at-home sleep study or an in-lab overnight study (polysomnography). At-home tests are common for straightforward suspected sleep apnoea and allow you to sleep in your own bed. In-lab studies capture more signals and are used for complex cases requiring deeper analysis. Your clinician will recommend the best option based on your symptoms and health history.
How do I prepare for my first sleep test to ensure accurate results?
Follow your normal routine as much as possible unless instructed otherwise by your clinic. Avoid late-day naps and limit caffeine after lunchtime. If attending an overnight lab, pack comfortable nightwear and toiletries. Aim for a typical night’s sleep rather than trying to ‘sleep perfectly’ to get the most useful data from your study.

What happens during an at-home versus an in-lab sleep study?
For an at-home study, you’ll take home a small device with sensors like a finger probe for oxygen levels, belts around the chest or abdomen, and a nasal cannula to measure airflow. You’ll wear it overnight and return it the next day. In an in-lab study, you’ll sleep overnight in a room resembling a hotel bedroom while a technician monitors multiple sensors on your scalp, face, chest, legs, airflow, and oxygen levels in real time.
Will the sleep test be uncomfortable or painful?
Sleep tests are not painful but some patients find the sensors mildly annoying at first. Most adjust within minutes and fall asleep normally once lights are off. If you’re sensitive to tape or adhesives, inform the clinic beforehand so alternative materials can be used where possible.
What should I do if I cannot sleep well during my sleep test?
Most studies still work even if you sleep less than usual since clinicians need only a minimum amount of recorded sleep time to interpret breathing patterns reliably. If you barely sleep, the clinic may recommend repeating the study. It’s important not to force yourself to sleep; staying calm usually leads to better results than stressing about the clock.